“TODAY THERE ARE riders on the road across the country. A patient is receiving blood from LifeBank now as we speak.”
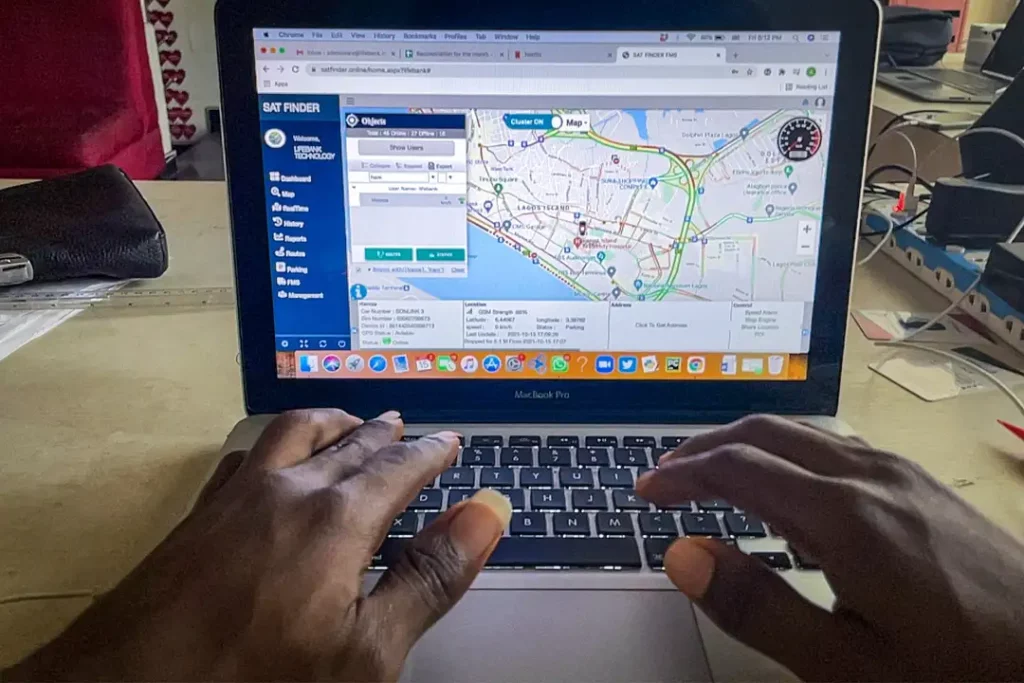
Ugochukwu Obiakor, the CEO of LifeBank Nigeria is describing what he sees on his computer screen, which shows in real-time LifeBank couriers’ exact location as they weave their way through the worst traffic Nigeria has to offer, delivering vital supplies from blood banks to hospitals.
He compares LifeBank’s service to Uber where once the order is made, a rider is dispatched to the blood bank nearest to the patient to pick up the required blood. “It takes around 45 minutes from the time we receive the order from the doctor to the arrival of the order at the patient’s bedside,” Obiakor says.
“If not for the access, I and my baby would not be alive.”
Temi Giwa-Tubosun, LifeBank founder
LifeBank was founded by Temi Giwa-Tubosun after she received a life-saving transfusion following the premature caesarean birth of her first child. She got the blood she needed in time because she was in a Minnesota hospital with a sophisticated blood supply chain.
“If not for the access, I and my baby would not be alive,” she told Nigeria’s Guardian newspaper. “If I’d given birth in Nigeria, one or both of us would not have survived it.”
That inspired her to create LifeBank, a technology-powered medical logistics company operating in Nigeria and Kenya, whose mission is to save lives. It does this by harnessing technology, including AI and blockchain, to connect hospitals to existing blood banks – filling gaps in infrastructure and making it all more efficient.
As riders race through the streets, carrying blood in WHO-certified cold boxes, they’re guided by the AI built into Google Maps. Their devices tell them the shortest and fastest route to the hospital. In a place like Lagos, famous for its nightmare traffic, these tools can make a life or death difference.
Upon receiving an order from doctors, LifeBank software matches it to the nearest supplier. A human then confirms with the bank that the blood exists and the rider speeds off. The company is developing a blockchain electronic ledger that will allow it to identify and track each bag of blood.
“This will enable anyone to scan the products with their smartphone and have a window pop up giving them all the product’s details,” Obiakor says. “For example, in the case of blood, date of donation and screening, blood group, pints, milliliters and so on. This will bolster safety and accountability.”
LifeBank has also successfully tested drone delivery in Ethiopia. Drones were programmed to pick up samples from blood banks and deliver them to hospitals without any human control. While still in early development, LifeBank hopes to expand drone delivery across Africa to help it deliver to hard to reach places.
“Healthcare practitioners are quite conservative in the use of technology.”
Ugochukwu Obiakor, CEO, LifeBank Nigeria
LifeBank works with more than 1,000 mostly private hospitals in Nigeria and has saved over 12,000 lives since launching in 2016, Obiakor says, adding there is potential to do much more.
“Healthcare practitioners are quite conservative in the use of technology,” he says. “What I’m seeing today is we’re struggling to get many healthcare providers and hospitals to use many of the tech platforms that we have, which would make it easier for us to serve them.”
As the need for oxygen grew during the Covid-19 pandemic, LifeBank began delivering that as well. Shortages and supply chain disruptions led LifeBank to start building a new AI-powered platform. Although still in development, it will predict when hospitals need to order key supplies such as oxygen, sutures, syringes or face masks.
“Using AI and historical data, we will be able to accurately predict for these hospitals their (level of) oxygen supply and what they need. We will be able to supply them ahead of time so they don’t get into a situation where they run out.”
Obiakor, who started his career as a pharmacist, is optimistic about the growing med-tech space and is exceedingly proud of the work so far. “We have made a real and quantifiable impact,” he says. “Even our riders report experiencing unforgettable moments. There’s this profuse gratitude when they arrive in hospitals just in time with the critical commodity that will save a patient’s life.”




